What symptoms of type 1 and type 2 diabetes: learn how to identify
Understanding the symptoms of type 1 and type 2 diabetes is critical to early diagnosis and treatment of this chronic disease. Diabetes is characterized by an increase in the level of glucose in the blood, which can lead to a series of serious complications, such as cardiovascular, kidney and vision problems.
Type 1 diabetes is an autoimmune disease in which the body’s own immune system attacks and destroys the insulin-producing cells in the pancreas. This results in a lack of production of insulin, the hormone responsible for regulating blood sugar.
Symptoms of type 1 and type 2 diabetes can include excessive thirst, frequent hunger, sudden weight loss, fatigue, blurred vision, and an increased need to urinate.Although these symptoms can be common to other conditions, it’s important to see a doctor if you experience them. suspected diabetes.
What is type 1 and type two diabetes?
Type 1 diabetes is an autoimmune disease in which the body’s own immune system attacks and destroys the insulin-producing cells in the pancreas, resulting in a lack of insulin production. Type 2 diabetes occurs when the body does not produce enough insulin or cannot use it properly.
Type 2 diabetes is more common and can be prevented or controlled with lifestyle changes, such as adopting a healthy diet and engaging in regular physical activity. It is essential to be aware of the symptoms and perform routine tests for an early diagnosis and adequate treatment of diabetes.
What is the difference between type 1 and type 2?
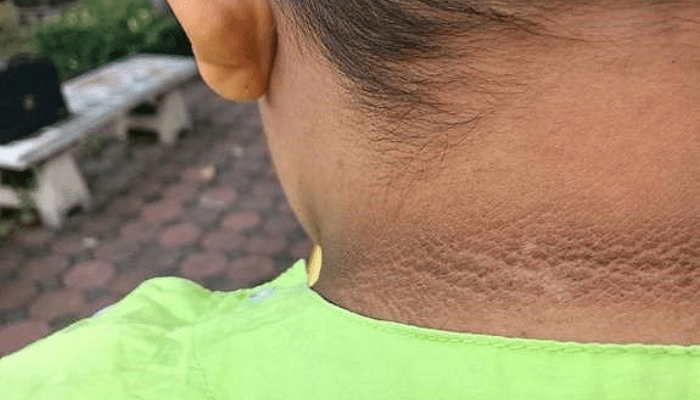
Some of the main differences between type 1 and type 2 diabetes are:
- Cause: Type 1 diabetes is caused by the destruction of insulin-producing cells in the pancreas by the body’s own immune system.
- Age of onset: Type 1 diabetes is more common in children and young adults, while Type 2 diabetes is more common in adults over age 40.
- Treatment: Type 1 diabetes is treated by administering insulin, usually through injections or insulin pumps.
- Prevention : Type 1 diabetes cannot be prevented as it is caused by a problem with the immune system.
- Complications: Both types of diabetes can lead to serious complications like cardiovascular, kidney and vision problems if not treated properly.
What is the difference between glucose and insulin?
Glucose and insulin are two key elements in controlling blood sugar and preventing diabetes. Glucose is a type of sugar that is found in the foods we eat, such as carbohydrates and sugars. When glucose is absorbed by the body, it is transported through the blood to the body’s cells, where it is converted into energy.
Insulin is a hormone produced by the pancreas that helps regulate blood sugar levels. When we eat, glucose is released into the bloodstream and the pancreas releases insulin to help transport the glucose to the body’s cells. Insulin helps open the body’s cells to allow glucose in, which helps lower blood sugar levels.
What is the difference between glucose and fasting blood glucose?
Glucose and fasting blood glucose are two terms frequently mentioned in diagnosing and monitoring diabetes. Glucose is a sugar present in the food we consume and is the body’s main source of energy.
The difference between glucose and fasting blood glucose can be summarized as follows:
- Glucose: sugar present in food and the body’s main source of energy. It can be measured at any time of the day, without the need for a prior fasting period.
- Fasting blood glucose: amount of glucose present in the blood after a fasting period of at least 8 hours. It is used in the diagnosis and monitoring of diabetes, with a normal value between 70 and 100 mg/dL. Values above 126 mg/dL in two consecutive tests indicate diabetes.
Maintaining fasting glucose and blood glucose levels within recommended values is important to prevent complications associated with diabetes, such as cardiovascular problems, kidney and nerve damage, among others.
What glucose value to go into a coma?
Hyperglycemia, i.e. excessive elevation of blood glucose levels, is a serious and potentially fatal complication of diabetes. When glucose levels exceed critical values, the body can enter a state of diabetic ketoacidosis, which can lead to diabetic coma.
The blood glucose value that can trigger a diabetic coma may vary according to each individual and their specific health conditions. In general, a blood glucose level above 600 mg/dL is considered critical and can lead to diabetic coma if not treated promptly.

Deixe um comentário